 According to a recent clinical review published in The Journal of the American Medical Association, promoting screening strategies and monitoring patients at extreme risk of melanoma is crucial for early detection and reducing the mortality rates of this highly prevalent cancer. As study author Vernon K. Sondak, M.D., chair of the Department of Cutaneous Oncology at Moffitt Cancer Center, said in a news release: “It is time to embrace the opportunity to decrease melanoma mortality through risk-stratified education and screening.”
According to a recent clinical review published in The Journal of the American Medical Association, promoting screening strategies and monitoring patients at extreme risk of melanoma is crucial for early detection and reducing the mortality rates of this highly prevalent cancer. As study author Vernon K. Sondak, M.D., chair of the Department of Cutaneous Oncology at Moffitt Cancer Center, said in a news release: “It is time to embrace the opportunity to decrease melanoma mortality through risk-stratified education and screening.”
The incidence of cutaneous melanoma continues to increase worldwide, with estimates showing a predicted 150,000 melanoma cases by the year 2030 in the United States alone. The U.S. Preventive Services Task Force skin cancer screening guidelines does not support screening for melanoma. However, this issue needs to be readdressed to adopt risk stratified screening, since early detection is crucial for improved disease outcome.
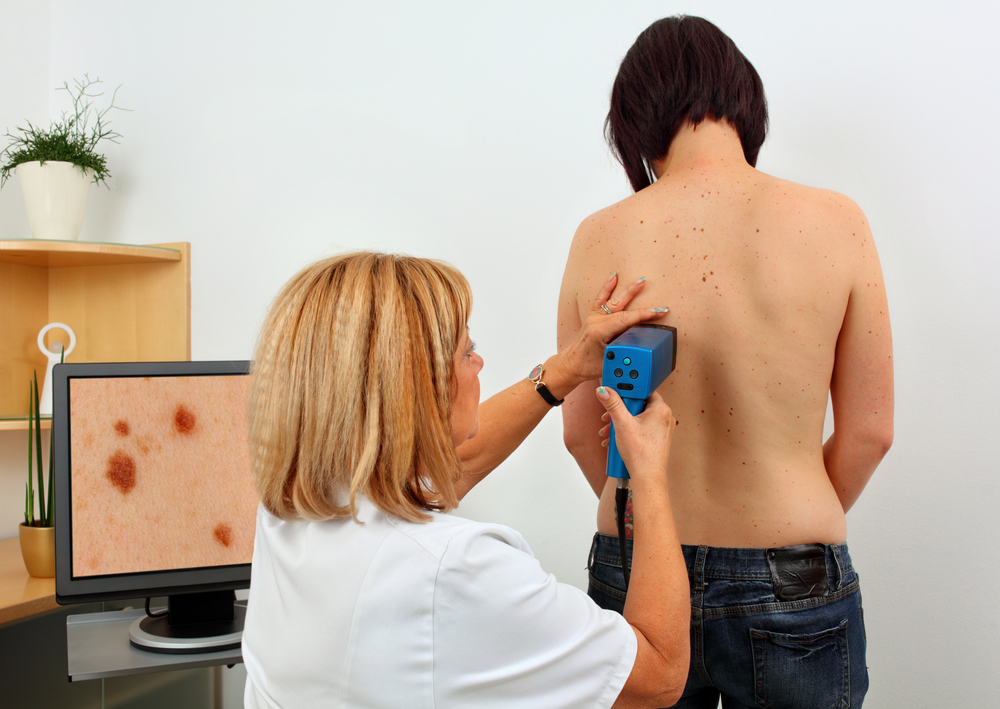
In the study titled “Risk-Stratified Screening for Detection of Melanoma,” physicians Vernon Sondak and L. Frank Glass, M.D from the Moffitt Cancer Center prospectively examined data of patients with melanoma recruited from the Sydney Melanoma Diagnostic Centre and Melanoma Institute Australia from 2006 to 2011. A total of 311 patients were examined for impact of dermoscopy and total-body photography (TBP) every 6 months. Patients considered as part of an extreme high risk population were further examined with sequential digital dermoscopy imaging (SDDI). All atypical lesions were excised.
After a median follow-up of 3.5 years, the physicians identified 75 primary melanomas, however, this was not related to an excessive number of unnecessary biopsies. Thirty-eight percent of these melanomas were detected with the TBP and 39% with the SDDI. Cumulative risk of developing a novel primary melanoma was 12.7% by year 2, with new primary melanoma incidence during the final 3 years of follow-up, half of that observed during the first 2 years.
Based on these findings, the physicians concluded that, “monitoring patients at extreme risk with TBP and SDDI assisted in early diagnosis of primary melanoma. Hypervigilance for difficult-to-detect thick melanoma subtypes is crucial.” This means that screening strategies should be focused on populations at high risk through the use of new imaging tools. Furthermore, clinicians should know how to effectively recognize early stages of melanoma.