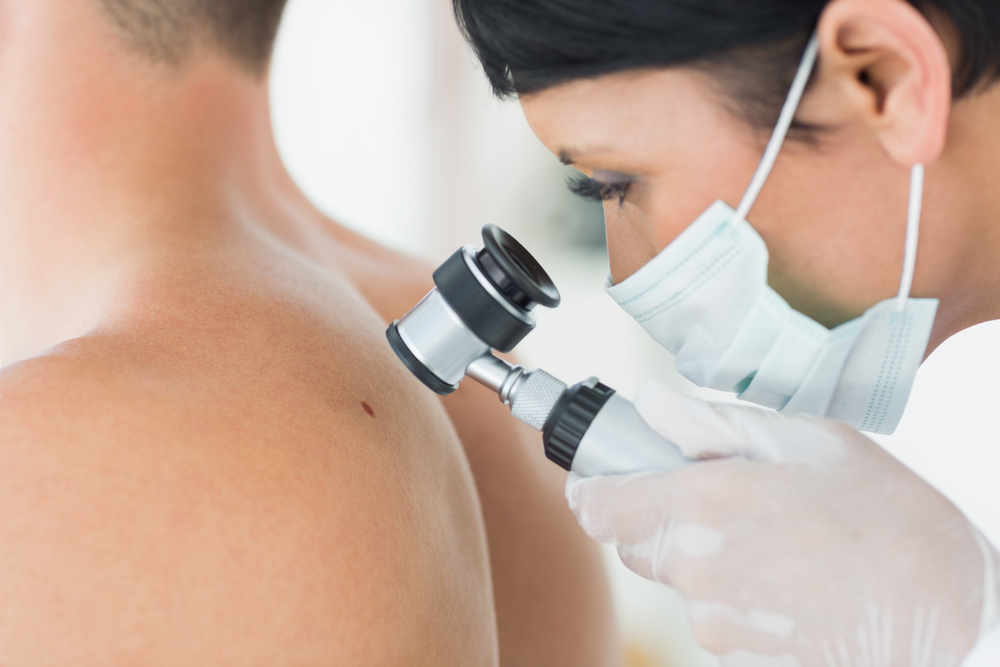
 In a new study entitled “PD-L1 marks a subset of melanomas with a shorter overall survival and distinct genetic and morphological characteristics”, published in the Annals of Oncology journal, a team of researchers led by Mario Mandalà, MD, Department of Oncology and Haematology, Papa Giovanni XXIII Hospital, Italy, have found that programmed cell death ligand 1 (PD-L1) is an independent prognostic marker in melanoma.
In a new study entitled “PD-L1 marks a subset of melanomas with a shorter overall survival and distinct genetic and morphological characteristics”, published in the Annals of Oncology journal, a team of researchers led by Mario Mandalà, MD, Department of Oncology and Haematology, Papa Giovanni XXIII Hospital, Italy, have found that programmed cell death ligand 1 (PD-L1) is an independent prognostic marker in melanoma.
PD-L1 is a cell surface molecule found in both T lymphocytes and tumor cells that plays a key role in suppressing immune responses, ultimately leading to tumor growth and malignancy.
Even though PD-L1 can be expressed in malignant melanoma, its clinical and biological function is still unresolved.
Using immunohistochemistry techniques, the researchers analyzed PD-L1 expression in 81 metastatic melanoma patients, observing that protein expression levels were correlated with clinical outcome.
The team used a human melanoma cell line and a mouse model of melanoma, finding that PD-L1 membrane positivity was an independent negative prognostic marker for this type of cancer.
Moreover, PD-L1 expression defined a subset of BRAF-mutated melanoma cells that have a highly invasive phenotype (leading to metastasis) and an increased capacity to grow into bigger tumors.
Through genetic profiling, the researchers could observe that melanoma cells expressing PD-L1 have an increased expression of genes connected to growth, activation, and invasion. However, after manipulating PD-L1 negative cells into expressing this receptor, no increased growth and motility properties were observed, which means that PD-L1 expression could be a downstream marker of the activation of an oncogenic pathway that characterizes a genetically different cell subset.
By evaluating paired melanoma samples, the team found that metastatic melanoma tissues expressed PD-L1 in significantly higher levels than primary lesions (40.3% vs. 14%), suggesting that the expression of this receptor is acquired throughout disease progression.
Regarding future research objectives, Dr. Mandalà discussed in a Medical Research interview “Our group is now focusing attention on the role of PD-L1 overexpression in melanoma patients treated with targeted oriented therapies. Another field of investigation is to understand whether PD-L1 is a predictive marker of PD-1 antibodies or it simply correlates with response. A third field of research is to understand the biological meaning of PD-L1 over expression in melanoma tissues with or without T cells infiltration in the microenvironment.”